Published: Sep 09, 2022
Meeting the needs of seniors in the digital age
Population ageing and urbanisation are two of the most significant demographic trends being observed in societies around the world today. Both of these trends have major implications for many areas of life, not least how we look at retirement.[1]
In 2018 the number of people aged 64 years and above surpassed the number of children under five years old for the first time in history, according to statistics from the United Nations. Meanwhile, the United States’ National Institute on Ageing expects that the global population of people aged 80 and older will more than triple from 126.5 million to 446.6 million between 2015 and 2050. In some Asian and Latin American countries, this cohort is expected to quadruple in size during the same period.

With more people living longer lives and fewer people entering the labour market, retirement savings and old-age pension systems are coming under significant strain. Poor economic conditions exacerbated by the Covid-19 pandemic have made the situation worse, according to a report from the Organisation for Economic Co-operation and Development (OECD).
Challenges brought about by population ageing extend beyond the economic sphere. Hence, there is a growing focus on population health so as to address healthcare needs as well as the Social Determinants of Health (SDOH) that are barriers to equity of health access. Various aspects under consideration are a greater emphasis on preventive health, a fundamental rethink of the use of urban spaces and infrastructure, and the active role that seniors can play in society.
In line with this, Singapore’s Ministry of Health (MOH) unveiled the “Healthier.SG” initiative this year. The initiative is intended to arrest rapidly increasing government healthcare expenditure (forecasted to triple to SGD 27 billion in 2030) and the increased utilisation of healthcare services brought about by the deteriorating health of Singaporeans due to ageing and the adoption of less healthy lifestyles (e.g., the number of Singaporeans who suffer from high blood pressure is up to 3 in 10 in 2020 from 2 in 10 in 2017).
This initiative comprises three main components:
- A designated Family Physician to oversee an individual’s overall care needs and who is linked to a public healthcare cluster managing the region the individual resides in
- A personalised Care Plan prescribed by the Family Physician with regular scheduled check-ups for better oversight and management of an individual’s health
- A support structure of Community Partners spearheaded by the public healthcare clusters to better support the needs of individuals under their coverage
Additionally, MOH has adopted an inclusive and holistic approach to ensure that our seniors are well cared for and as active as possible throughout their retirement years.
Supporting seniors in the three Cs — Care, Contribution, and Connectedness
Care:
MOH promotes a Senior Care Centre Service Model where seniors can receive active ageing, befriending, and referral-to-care services. This also benefits seniors who live independently as it allows them to receive continuous support to engage in physical (e.g. exercise) and virtual activities, widen their social circles, and stay physically well and mentally alert to stave off physical frailty and the onset of dementia. Befriending is an essential activity to keep seniors engaged, especially those living alone.
Contribution:
Many seniors want to contribute meaningfully to society through learning, volunteerism, and continued employment. These activities allow seniors to interact with younger Singaporeans and impart their life experiences, skills, and values, thereby building inter-generational bonds.
Connectedness:
Urban spaces are generally not senior-friendly. A recent paper entitled Planning for Age-Friendly Cities points out that societies tend to segregate seniors in residential care units, retirement villages, and nursing homes. This restricts their interactions with society at large and is detrimental to their overall well-being.
Inclusive age-friendly cities built around the concepts of “ageing-in-place” and “active ageing”1 run counter to this. The World Health Organization (WHO) defines active ageing as “the process of optimising opportunities for health, participation, and security in order to enhance quality of life as people age”. An age-friendly city benefits everyone and treats seniors as active, valued participants in their communities and the economy.

MOH has put in place measures to support seniors to age-in-place by increasing access to diverse home and community-based care options within an inclusive environment.
A Community Care apartment pilot i.e. an integrated housing-cum-care model centred around public housing units integrated with adjoining facilities such as a primary care polyclinic, a supermarket, a community centre, and a food centre integrated within the same estate, saw strong demand. There is great potential to expand this to the private sector and also to offer more innovative assisted living models.
The rise of gerontechnology
Rethinking old age in the context of an increasingly technology-saturated world has led to the rise of gerontechnology, an interdisciplinary field focused on using advances in technology to maximise the independence of seniors and promote the overall well-being and quality of life of these individuals as well as that of their families and caregivers.
Gerontechnology addresses challenges associated with old age, including functional declines, loneliness, depression, cognitive impairment, and social isolation, among others.
Telehealth, one branch of gerontechnology, has proven benefits in senior care. CareLine, for example, is a 24/7 personal care telephone service that provides tele-befriending and emergency response services to seniors who are living alone or are frail, thereby helping these seniors to keep safe at home. Call agents are trained to converse in the vernacular. Supporting 17,000 vulnerable seniors, CareLine receives 30 calls a month from seniors requiring emergency services. To right-site care, call agents are trained to triage seniors’ conditions after a distress episode and provide remote assistance or activate non-urgent in-person assistance through nearby community providers.
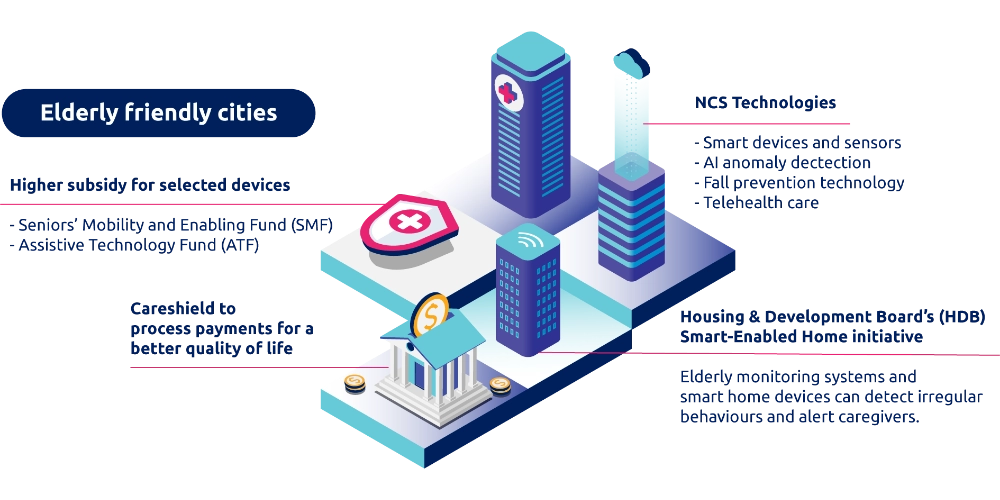
NCS sees a potential for this service to be scaled to cater to the needs of more tech-savvy seniors through an app that features a befriending chat service that also incorporates an AI-based symptom checker to help triage seniors’ conditions and provide remote assistance or activate non-urgent in-person assistance through nearby community providers. Going one step further, this app could be linked to smart sensors installed in the seniors’ homes that monitor their behaviour and activity routine so as to automatically detect and activate assistance should deviations be detected. This is a realistic aim given the Housing & Development Board’s (HDB) Smart-Enabled Home initiative which aims to improve daily living in HDB homes through the use of commercial smart home devices.
Tele-health, in other forms, continues to evolve, offering an ever-increasing range of services from virtual consultations to prescription drug refill authorisations to remote care services that include remote diagnostics and health monitoring.
Assistive technology, on the other hand, can help seniors with reduced mobility, visual and hearing impairments, dementia, and other conditions that undermine their independence. Examples include screen reading software which converts text-to-speech or braille, screen magnification software, amplified telephone equipment, memory aids, and personal emergency response systems which automatically alert caregivers when a senior is in danger.
Inching closer towards an age-friendly society
“Singapore’s healthcare institutions, especially those in public healthcare, are already at a certain level of maturity of technological advancement compared to most countries,” says Jim Lim, Healthcare Sector Lead at NCS. Moving forward, there are many opportunities to digitalise the long-term and senior care sectors with new technologies like artificial intelligence (AI), robotics, and 5G to support more integrated care and the realisation of an age-friendly society.
NCS is working to innovate solutions to support “ageing-in-place” and senior independent living to enhance the quality of life of seniors. For example, a cloud-based senior independent monitoring solution called CARECONNECT was piloted by NCS Australia.
NCS’s emphasis on senior safety led us to develop a fall prevention solution which uses state-of-the-art video analytics, 5G, and deep learning algorithms to anticipate and prevent seniors from falling. The solution is currently being piloted in a senior care institution in Singapore.
Moreover, NCS’s strong focus on robotics has led to the development of a robotic nursing assistant, aptly called Florence, to provide assistance to ward nurses through patient bedside interactions and vital signs measurement. Other robotic solutions offered by NCS support operations like item delivery and tele-presence solutions such as video consultations and engagement and interaction with seniors.
There is still much to be done to build an age-friendly society that allows people of all ages to flourish. Strategic planning coupled with the application of suitable technologies in the correct context and at the right price, will ensure we meet the evolving needs of an ageing population in a sensible and sustainable manner.
[1] Global Age-Friendly Cities: A Guide, World Health Organization (2007), https://www.who.int/ageing/publications/Global_age_friendly_cities_Guide_English.pdf



